- Print this page
- Share this page
Guidelines for the provision of relevant services have been published
SIRA has published the Guidelines for the Provision of Relevant Services (Health and Related Services), which apply to relevant service providers providing services in the NSW workers compensation and CTP (for accidents on or after 1 December 2017) schemes.
The following sections of the guidelines apply to allied health practitioners providing relevant services in the workers compensation scheme:
- Part 1: Code of conduct (Non SIRA-approved allied health practitioners only)
- Part 2: Requirements for telehealth services
- Part 5: Billing requirements for the provision of relevant services under the workers compensation legislation
- Part 6: Invoicing requirements for relevant services under the workers compensation legislation (excluding pharmaceutical services)
This web page has been updated for consistency with the Guidelines.
Introduction
Allied health practitioners have an important role in the NSW workers compensation scheme. You are engaged to provide specialised expertise to assess a worker’s capacity and any barriers to recovery at work, and to provide evidence based treatment with a focus on return to work to optimise worker recovery.
This guide will help you understand what to do and what to expect when delivering services for a patient with a worker’s compensation claim. It outlines your obligations under workers compensation legislation, and provides practical advice to help get the best possible outcome for the worker.
The guide also explains the roles of the other people in the worker’s support team, including the employer, doctor, insurer, approved workplace rehabilitation provider, and any other allied health practitioners involved.
Most injured workers take little or no time off work after sustaining an injury. For those that do, the vast majority (more than 80 per cent) return to and recover at work within the first 13 weeks.
Advice and direction in this guide is based on a strong body of research and evidence about the health benefits of good work. It explains how returning to and where possible, recovering at work after an injury, can promote healing and facilitate recovery.
Workers compensation in NSW
The NSW workers compensation scheme operates under the Workers Compensation Act 1987 (1987 Act) and the Workplace Injury Management and Workers Compensation Act 1998 (1998 Act), and associated Regulation. It provides no-fault protection to workers and their employers following a work related injury or illness.
The State Insurance Regulatory Authority (SIRA) is the government organisation responsible for regulating the NSW workers compensation scheme.
SIRA licenses insurers in NSW, including:
The Workers Compensation Nominal Insurer (Nominal Insurer) is a statutory legal entity constituted by section 154A of the 1987 Act. Under the Act the Nominal Insurer is taken to be a licensed insurer and is responsible for managing the operation of the Workers Compensation Insurance Fund.
icare (Insurance and Care NSW) is a NSW Government agency that acts for the Nominal Insurer and provides services for authorities that provide insurance and compensation schemes in NSW. Those authorities are the:
- Workers Compensation (Dust Diseases) Authority
- Lifetime Care and Support Authority of New South Wales
- Sporting Injuries Compensation Authority
- NSW Self Insurance Corporation (SICorp).
Self-insurers are SIRA approved employers who manage their own workers compensation claims.
Specialised insurers hold a restricted licence to provide workers compensation insurance for a specific industry, class of business or employer.
Regardless of which type of insurer is involved, they all have an obligation to support workers and employers during the recovery process and manage the claim to ensure entitlements are received.
Workplace injury management
The 1998 Act identifies specific responsibilities for insurers, employers, and treatment practitioners to encourage a safe, timely and sustainable recovery at/return to work.
Injury management is an integrated process involving four components within a biopsychosocial framework. Injury management is an integrated process involving four components which consider the biological, psychological, behavioural and social (biopsychosocial ) factors as they relate to an individual worker.
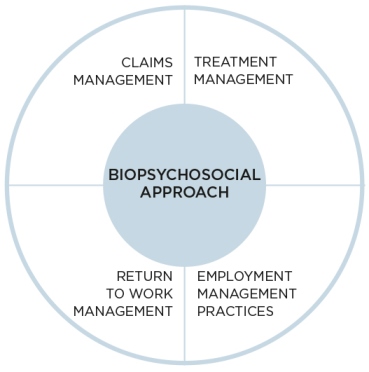
Claims management is performed by the insurer. This includes determining liability for the claim, exchanging information and planning with other members of the support team. It also means coordinating service provision and payment for services, and helping the employer meet their obligation to provide suitable work options for the worker.
Treatment management is performed by the nominated treating doctor in collaboration with all members of the worker’s treatment team, including allied health practitioners All treating providers need to be aligned in regard to the setting of goals with the worker. Effective communication between all parties is essential to ensure a coordinated approach and deliver these goals.
Return to work management is a team effort. It involves coordinated planning and support by everyone in the team to enable the worker to recover at/return to work.
Employment management practices are developed by the employer to prevent and manage workplace injuries.
The evidence for recovering at work
Research shows that:
- for most people with a work-related injury, time off work is not medically necessary
- an unnecessary delay in returning to work is often associated with delayed recovery – the longer a worker is away from work, the less chance they have of ever returning1, 2
- staying active after injury reduces pain symptoms and helps workers return to their usual activities at home and at work sooner1, 2
- working helps workers stay active which is an important part of their treatment.1, 2
The support team
In the workers compensation scheme, returning to and recovering at work is a managed process involving a multidisciplinary team.
Evidence suggests that shared goals, communication and cooperation among the support team is critical in improving clinical and occupational outcomes for the worker.3
Success depends on the integration of sound clinical, workplace and insurance claims management, as well as agreement across the team about the worker’s goals and progress. So, it’s important you understand the role of others in the support team.
The team includes the employer, insurer case manager, doctor, a workplace rehabilitation provider (if required) and you. Each member has an important role to play in the worker’s recovery and these are outlined below.
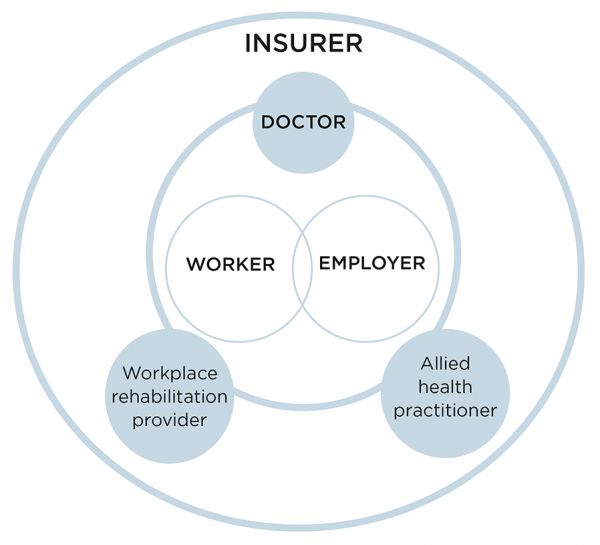
The worker’s role is to focus on their recovery. They should aim to stay at work in some capacity, or return to work as soon as possible. They must notify their employer of their injury or illness as soon as possible after it has occurred. They are also required to maintain a current SIRA certificate of capacity and provide a copy to their employer and/or insurer.
The worker has the right to choose their treating allied health practitioner. The chosen practitioner however must meet the requirements and conditions outlined in the guidelines for approval of allied health practitioners in order to deliver any treatment services to the worker.
The Guidelines for workplace return to work (RTW) programs outline the employer’s obligations to support recovery at work. Employers must offer suitable work, where reasonably practicable, even when the claim is under dispute under s41 Workplace Injury Management and Workers Compensation Act 1998.
This work should be as close as possible to the worker’s normal duties in order to maximise their recovery. If the worker is employed by a large employer, there may be a return to work coordinator, whose role is to assist the worker with their recovery/return to work.
The greater the employer’s ability to accommodate their worker while they recover, the less likely it is that they will need time away from the workplace as a result of their injury.
RTW is improved by contact between the worker and the workplace. The employer can assist by:
- providing information about the workplace, the worker’s usual job and available short term suitable work options and support for recovery at work
- discussing any risks or barriers that may have an impact on the worker’s recovery
- developing a written recover at work plan to ensure the worker’s recovery progresses as expected and that they receive adequate support in the workplace.
Note: An employer cannot terminate a worker’s employment because of a work-related injury within six months of the worker first becoming incapacitated for work.
The role of the insurer is to coordinate and manage a workers claim, including injury management and recovery at work activities. The insurer appoints a case manager who coordinates all aspects of the worker’s compensation claim. The insurer maintains regular communication and engagement with all the stakeholders to coordinate support.They are the primary contact for the worker and support team. It is their responsibility to establish positive working relationships with all key parties.
After receiving notification of a work-related injury, the case manager makes early contact with the worker, employer and support team in order to determine the assistance required.
The case manager helps the employer meet their legal obligations. They also may arrange assessments or services for the worker, authorise payment for ‘reasonably necessary’ medical expenses, and determine the worker’s entitlement to weekly compensation payments.
You are encouraged to discuss the worker’s capacity with both the doctor and the case manager. To facilitate case management, you should respond to telephone calls from the case manager at the earliest opportunity.
The nominated treating doctor will assess, diagnose, and recommend treatment, supporting the worker to recover at work where possible and contributing to RTW planning in collaboration with the worker and support team. They will also assess their capacity for work and support their recovery. Selected by the worker, the doctor is usually their general practitioner.
The doctor has a key role in the worker’s recovery and rehabilitation. They:
- provide the worker with a completed initial certificate of capacity and may also issue subsequent certificates of capacity
- act as the primary communicator for treatment and the injury management plan
- are authorised by the worker to provide relevant information to the employer, insurer and other parties involved in the management of the injury.
The Guidelines for the Provision of Relevant Services (Health and Related Services) make it a requirement for allied health practitioners to work collaboratively and communicate in an effective and timely manner with members of the injured person’s support team about the injured person's injury, treatment, and recovery.
Workplace rehabilitation providers deliver specialised services to help workers recover at/return to work.
Workplace rehabilitation services are usually delivered at the workplace and may provide specialised expertise to assist:
- In tailoring support for the worker with consideration to the biopsychosocial factors that may influence a recovery and return to work
- An employer to identify suitable work and other workplace adjustments to accommodate the individual needs of a worker, based on the principles of good work
- A worker to obtain work with a new employer including assessment to identify suitable employment options, job seeking assistance and facilitating access to programs to secure new employment
- Support from a provider is in addition to that generally available from an employer, and delivered when additional support is needed, or return to work is not straightforward
While it is usually the employer or insurer who makes the decision on which approved workplace rehabilitation provider will be used in each situation, the worker must be consulted on the decision and given the opportunity to refuse or request a different provider.
The insurer is responsible for engaging the workplace rehabilitation practitioner and paying for their services.
As the allied health practitioner, your primary objective is to support the worker to optimise their recovery and return to work. This is generally achieved through evidence‑based clinical intervention and management.
The worker will look to you for information about their condition and recovery. Your role may involve:
- setting expectations from the first consultation regarding their recovery at/return to work, active participation in recovery, planning and treatment
- conducting a detailed assessment and (where applicable) providing information to inform and/or confirm diagnosis and treatment strategies. Where a diagnosis is not clear, you should provide a provisional diagnosis and explain your reason(s) for this
- obtaining information from the insurer and/or employer to assist with goal setting and tailoring of treatment interventions
- providing information to the support team regarding the worker’s progress and capacity for work
- educating the worker about the health benefits of good work
- improving the worker’s independence and participation in their home and community
- completion of certificates of capacity where appropriate and within your scope of practice (physiotherapists and psychologists only).
Note: Your role does not include advocating for the worker in relation to the management of their claim, litigation or other compensation processes.
Other health practitioners may be involved in the management of the worker’s injury/condition and may help you facilitate the worker’s recovery by:
- conducting a detailed assessment of the worker and sharing information to inform and/or confirm diagnosis and the treatment strategy
- providing treatment to improve the worker’s capacity for work
- providing recommendations about the worker’s progress and their capacity for work
- collaborating with other members of the support team to ensure the team is working towards shared goals and providing consistent messaging to the worker
Independent consultants are experienced in the assessment and treatment of workplace injuries. They provide an independent peer review of allied health treatment in the workers compensation system.
Only SIRA-approved independent consultants can undertake these reviews. Find a list of approved independent consultants here.
An injury management consultant is a registered medical practitioner approved by SIRA and experienced in occupational injury and workplace based rehabilitation.
They work with the doctor and other members of the support team to negotiate a way forward in cases where there are barriers that are delaying, or have the potential to delay, a worker’s recovery at/return to work. The injury management consultant may liaise with you as part of this process.
Independent medical examiners are registered medical practitioners with qualifications relevant to the worker’s injury.
The worker, their legal representative, or the insurer can request an independent medical examiner to review medical information and/or examine the worker, when information from the doctor is unavailable, inadequate, or inconsistent, or when the insurer has been unable to resolve issues after discussion with the doctor.
SafeWork NSW inspectors help employers and employees understand their rights and obligations under work health and safety, workers compensation and injury management legislation. They may be involved to review an employer’s RTW system to facilitate the offer of suitable work.
A worker can request assistance from SafeWork NSW if their employer has not provided suitable work.
Inspectors also have the power to issue an Improvement Notice should they believe an employer has contravened the requirement to provide suitable employment following a workers compensation claim. For more information, refer to the SafeWork NSW website.
Communicating with the support team
Each member of the support team has an important role to play in the worker’s recovery.
Clear communication and collaboration with others in the support team is essential to:
- understand the worker’s capacity and needs
- identify any barriers or risks to recovery and effective strategies to address these issues
- develop shared goals and recovery expectations
- ensure the worker receives consistent messages from all support team members
- ensure the right services are provided at the right time.
Issues may arise during the life of the claim that you may wish to discuss with members of the support team. Some examples include, but are not limited to:
- if the worker is repeatedly late or does not attend their appointment(s)
- if you are considering a referral to a specialist, workplace rehabilitation provider or independent consultant
- if the doctor wants you to continue treatment and you don’t consider further treatment appropriate
- if the doctor is a barrier to upgrading the worker or is delaying the process
- if your assessment of work capacity differs from what the doctor has certified
- if the worker needs to be directed to an alternate allied health practitioner
- if the worker has been certified for pre-injury duties but you believe they will require ongoing treatment for a brief period to remain at work.
Delivering services in the NSW scheme
In the NSW workers compensation scheme, allied health practitioners are classified under two categories:
- SIRA approved allied health practitioners
- non SIRA approved allied health practitioners
These categories are based on the practitioner’s discipline of practice and registration (or membership) as a health practitioner.
Some differences exist between these two categories in terms of:
- processes for approval of services, and
- fees payable
- application of the code of conduct in Part 1 of the Guidelines for the Provision of Relevant Services (Health and Related Services)
These are detailed throughout the guide.
SIRA approved allied health practitioners
Some allied health practitioners must be approved by SIRA before providing services in the NSW workers compensation scheme. The approval period is for three years. These practitioners include:
- chiropractors, osteopaths, physiotherapists, and psychologists. These practitioners must have general registration with the Australian Health Practitioner Regulation Agency (AHPRA)
- exercise physiologists who are accredited with Exercise & Sports Science Australia (ESSA)
- counsellors who are:
- full clinical members of the Psychotherapy and Counselling Federation of Australia (PACFA), or
- mental health social workers accredited with the Australian Association of Social Workers (AASW), or
- level 3 or 4 members of the Australian Counsellors Association (ACA)
SIRA approved allied health practitioners must satisfactorily complete a training program, meet and adhere to the conditions of approval, set out in the workers compensation guidelines for approval of treating allied health practitioners, and apply and be granted approval by SIRA before they can deliver services in the NSW workers compensation scheme.
SIRA approved allied health practitioners must also comply with the following parts of the Guidelines for the Provision of Relevant Services (Health and Related Services):
- Part 2: Requirements for telehealth services
- Part 5: Billing requirements for the provision of relevant services under the workers compensation legislation
- Part 6: Invoicing requirements for relevant services under the workers compensation legislation (excluding pharmaceutical services)
Note: Clinical neuropsychologists assessing workers in the NSW workers compensation scheme do not require SIRA approval.
There is a searchable list of approved practitioners on our website. If approved, allied health practitioners have their name and contact details added to this list.
It is the responsibility of the practitioner to notify SIRA (in writing) within 14 calendar days if any of their listed details change.
Once approved, practitioners are provided with a SIRA workers compensation approval number. This number is specific to the individual and cannot be used by any other person.
Note: Each practitioner only requires one approval number per discipline practised. This can be used at each location they work.
If an allied health practitioner does not meet or adhere to the requirements and conditions of approval outlined in the Workers Compensation Guideline for approval of treating allied health practitioners , SIRA may decline, suspend or revoke their approval.
Non SIRA approved allied health practitioners
Non SIRA approved allied health practitioners include all other allied health disciplines that do not require SIRA approval.
Non SIRA approved allied health practitioners should adhere to the principles and procedures set out in this guide, except where the guide specifies the procedure only applies to SIRA approved allied health practitioners.
Non-SIRA approved allied health practitioners must also comply with the following sections of the Guidelines for the Provision of Relevant Services (Health and Related Services):
- Part 1: Code of conduct
- Part 2: Requirements for telehealth services
- Part 5: Billing requirements for the provision of relevant services under the workers compensation legislation
- Part 6: Invoicing requirements for relevant services under the workers compensation legislation (excluding pharmaceutical services)
Allied health practitioners precluded from delivering services in the scheme
Allied health practitioners whose registration is limited or subject to any conditions as a result of a disciplinary process, are precluded from delivering any treatment services to NSW workers.
Other conditions/limitations on an allied health practitioner’s registration, unrelated to a disciplinary process will be considered on a case-by-case basis.
Practitioners with conditions on their registration are encouraged to contact us on 13 10 50 to determine their eligibility for SIRA approval prior to completing the online training program.
Interstate allied health practitioners
Interstate allied health practitioners providing treatment services to a NSW worker outside of NSW do not need to be approved by SIRA. They are not required to undertake the NSW allied health practitioner online training either.
However, every service practitioner must adhere to the NSW workers compensation scheme requirements. This means:
- meeting the conditions for approval outlined in the guidelines for approval of treating allied health practitioners (excluding completion of the online training, however SIRA would encourage the completion of this training by interstate practitioners to assist with their knowledge of delivering services in the NSW workers compensation system)
- complying with the following sections of the Guidelines for the Provision of Relevant Services (Health and Related Services)
- Part 1: Code of conduct
- Part 2: Requirements for telehealth services
- Part 5: Billing requirements for the provision of relevant services under the workers compensation legislation
- Part 6: Invoicing requirements for relevant services under the workers compensation legislation (excluding pharmaceutical services)
- submitting allied health recovery requests for the prior approval of treatment services, and
- adhering to all policies and procedures set out in this guide
Training in the workers compensation scheme
To build capability in the NSW workers compensation scheme, there is an online allied health practitioner training program.
All allied health practitioners must complete this training to improve their ability to navigate the workers compensation scheme and manage their compensable patients effectively. For allied health practitioners seeking SIRA approval satisfactory completion of the training is mandatory. This program is completed at the practitioner’s own cost.
All allied health practitioners are encouraged to complete this training to improve their ability to navigate the workers compensation system and manage these clients effectively. This program is completed at the practitioner’s own cost.
Supervision of SIRA requirements
SIRA recognises that the majority of allied health practitioners providing services in the scheme are doing the right thing. However, SIRA may need to deal with practitioners with a pattern of poor practice who have not responded to opportunities provided by SIRA to correct those practices.
SIRA will ensure actions taken in response to non-compliance with SIRA requirements are appropriate, proportionate, and effective. Actions that could be taken in response to non-compliance may include:
- SIRA may contact the practitioner to discuss the matter, help identify the causes of non-compliance, and provide support and education to remedy any gaps in understanding.
- SIRA may write to the practitioner, informing them where they are failing to meet requirements, how to comply with requirements, and that SIRA has the power to give a direction if requirements are not complied with.
Practitioners will be given the opportunity to make submissions about their behaviour and why further compliance activity is not warranted. It is expected that most matters will be remedied in discussion with the provider.
If non-compliance continues, SIRA may suspend or revoke SIRA approval, where relevant, or issue a direction under section 26D of the State Insurance and Care Governance Act 2015. A direction could include requiring the provider to take certain action or, if there is a risk of harm to injured workers or the schemes, to suspend or exclude the practitioner from providing services in the CTP and WC schemes.
In general, SIRA will not investigate concerns about an allied health practitioner’s clinical or professional conduct or intervene in individual clinical decision-making. If SIRA considers there is a potential risk to an injured worker’s health or welfare, SIRA may refer the matter to an appropriate body for investigation, such as the Health Care Complaints Commission, or the Health Professional Councils Authority.
Providing services to workers
Allied health practitioners make a significant contribution to improving health and achieving positive recovery at/return to work outcomes for workers, particularly in the early stages after injury.
All allied health practitioners in the NSW workers compensation scheme must adopt the principles of the Clinical Framework for the Delivery of Health Services.
Developed by the Transport Accident Commission and WorkSafe Victoria. The framework reflects the most contemporary approach in the delivery of treatment, and outlines expectations when treating an individual with a compensable injury.
The five principles of the clinical framework are:
- Measure and demonstrate the effectiveness of treatment.
- Adopt a biopsychosocial approach.
- Empower the injured person to manage their injury.
- Implement goals focused on optimising function, participation and return to work.
- Base treatment on the best available research.
The framework is supported by the Australian Physiotherapy Association, the Australian Psychological Society, the Australian Chiropractors Association , Osteopathy Australia, Chiropractic Australia and Occupational Therapy Australia.
Conflict of interest
You need to consider conflicts of interest when providing services in the NSW workers compensation scheme.
A conflict of interest is a situation where you could be influenced (or perceived to be influenced) by a personal interest when carrying out your allied health practitioner duties.
For example this could occur if you have competing professional and personal interests that make it difficult for you to fulfil your duties impartially, or improperly influence your performance of these duties.
Allied health practitioners must be aware of their responsibilities and requirements regarding conflicts of interest.
- SIRA approved allied health practitioners: must not ask for or accept any inducement, gift, or hospitality from individuals or companies, or enter into arrangements that could be perceived to provide inducements, that may influence, or be seen to influence, their ability to provide treatment to the worker that will best meet their needs (for example, offering or accepting financial incentives for referral of workers); and declare any real, perceived or potential conflict of interest to the referrer and worker at time of referral or, if a conflict or potential conflict of interest arises after referral, as soon as it arises (see 2.2.6 and 2.2.7 of the Workers Compensation Guideline for Approval of Treating Allied Health Practitioners.
- Non SIRA approved allied health practitioners: must identify perceived, potential, and actual conflicts of interest and manage them to ensure services provided best meet the needs of injured people. Where there is an actual conflict, declare it to the injured person concerned, the referrer and the insurer concerned, as per refer to Part 1.2 g) in the code of conduct contained in the Guidelines for the Provision of Relevant Services (Health and Related Services).
When assessing the presence of a conflict of interest, you should consider:
- personal, professional or business-to-business financial gain or benefit
- existing practitioner, client or familial relationships
- businesses in which you, your friends or family have an interest
- a worker’s location (such as availability of services in rural and remote areas)
- disclosing sensitive or confidential information gained through employment to another organisation
- any financial or other personal interest that could directly or indirectly influence or compromise you when performing services.
Declarations of conflicts of interest to insurers by SIRA approved allied health practitioners will be assessed by the insurer on a case-by-case basis.
If the insurer decides you can deliver services to the worker, it is your responsibility to inform the worker of the real, perceived or potential conflict of interest and to document it in the worker’s notes.
If you are dissatisfied with the insurer’s decision, you should follow the complaints process outlined in the workers compensation guidelines for the approval of treating allied health practitioners.
When you receive a referral
When you receive a referral for allied health services, contact the insurer before your first appointment with the worker to confirm:
- their claim has been accepted
- they are eligible for payment of medical and related expenses
- the insurer agrees treatment is reasonably necessary
Physiotherapists, chiropractors and osteopaths do not require a referral to commence treatment. All other allied health practitioners including SIRA approved psychologists, accredited exercise physiologists, and counsellors require a referral from the nominated treating doctor before treatment can commence.
Insurer approval for allied health treatment may have a time limit.
That’s why it’s important you confirm the worker’s eligibility for paid medical (and related) expenses with the insurer before your initial consultation. You may not be paid if you fail to do so. Contact the insurer via phone or email as a first step.
If the insurer does not agree to fund treatment at the time of referral, or if the worker’s eligibility for medical and related expenses ends, the costs of any treatment provided thereafter will be the responsibility of the worker.
In the event a claim is later accepted, the insurer may be responsible for payment of services already paid for by the worker. In this situation, if the fee charged to the worker exceeded the maximum gazetted rates, the insurer may seek to recover amounts paid above the maximum gazetted fees from you.
You should have a clear arrangement in place with the worker to ensure they notify you of any changes to their eligibility. If there is a change in the worker’s eligibility, the insurer must inform them directly. It is recommended that the insurer also informs any treating allied health practitioner of the change at the same time.
Workers can receive any reasonably necessary treatment and services within 48 hours of the injury occurring without pre‑approval from the insurer.
In some instances, SIRA approved practitioners are not required to obtain prior insurer approval for service provision. This is designed to help the provision of timely treatment to support the worker’s recovery at/return to work. Practitioners should however note they still need to confirm with the insurer prior to the initial consultation if the worker is eligible for services (as stated in the previous section on eligibility)
For a full list of exemptions from prior approval refer to the Guidelines for claiming workers compensation. These exemptions do not apply to exempt categories of workers (police officers, fire fighters, paramedics).
Non SIRA approved practitioners must obtain insurer approval prior to delivering any treatment services to a worker.
Interstate practitioners who are not SIRA approved must obtain insurer approval prior to delivering any treatment services to a worker.
Where a worker is eligible for medical and related treatment expenses for a workers compensation claim, you are unable to bill under the Medicare Benefits Schedule. You must bill the relevant insurer.
The Medicare Benefits Schedule states:
Medicare benefits are not payable where the medical expenses for the service are for a compensable injury or illness for which the patient’s insurer or compensation agency has accepted liability.
Setting expectations at the first assessment
You and the worker should discuss and formulate an expectation of recovery as soon as possible after injury.
Discuss self-management strategies and reassure the worker that most people recover quickly after an injury. Explore the worker’s expectations of recovery and work. It is recommended that a psychosocial risk screening tool such as the Orebro Musculoskeletal Pain Screening Questionnaire (Short form) (OMPSQ 10) be completed by the worker at, or before your initial appointment with them to identify any barriers to recovery to guide these discussion and appropriate self-management.
As an allied health practitioner, there are certain requirements you must meet when communicating with and submitting documentation to other members of the support team.
It is expected that you communicate with the relevant parties as part of the initial assessment process. You should discuss the worker’s management and formulate common recovery at/RTW and treatment goals. This includes:
- communicating with the nominated treating doctor to discuss diagnosis, current and proposed treatment and how the treatment will aid recovery and build capacity for work
- communicating with the referrer (if not the doctor)
- having meaningful dialogue with the worker’s employer or return to work coordinator and workplace rehabilitation practitioner (if involved) to ensure you understand the worker’s pre-injury duties and the availability of suitable work
- discussing your expectations of the worker’s capacity
- communicating with the insurer if appropriate.
Pre-existing or co-existing non-compensable health conditions
The worker’s recovery at/return to work may be compromised when other health conditions are present.
Treatments for a compensable condition may be hindered, delayed or medically inappropriate due to pre-existing or co-existing non-compensable health conditions.
It is important the compensable condition is clearly stipulated by the insurer, not only for the worker and employer, but also for treatment practitioners who may otherwise unknowingly provide services unrelated to the compensable injury.
If you identify barriers to recovery due to a health condition that is not directly related or attributable to the compensable injury or illness, make sure the doctor and worker are aware of the issues. The doctor can then follow up regarding appropriate management which may include accessing services via Medicare, a private health fund, and so on.
If you feel it is appropriate to talk to the insurer about any non-compensable issue impacting the recovery of the compensable injury, you should seek consent from the worker to do so.
It may not be necessary to disclose all details, but rather flag the existence of a barrier and advise that management will occur concurrently with the compensable injury or illness.
Reasonably necessary treatment services
Before approving or paying for a medical, hospital or rehabilitation treatment or service, an insurer must determine, based on the facts of each case, that the treatment or service:
- is reasonably necessary, and
- is required as a result of the work-related injury/illness.
When considering the facts of the case, the insurer should understand that:
- what is determined as reasonably necessary for one worker may not be reasonably necessary for another worker with a similar injury
- reasonably necessary does not mean absolutely necessary
- although evidence may show that a similar outcome could be achieved by an alternative treatment, it does not mean that the treatment recommended is not reasonably necessary.
In most cases the above points should be sufficient for an insurer to determine what is reasonably necessary. Where the insurer remains unclear on whether a treatment is reasonably necessary, the following factors may be considered:
- the appropriateness of the treatment
- the availability of alternative treatment
- the cost of the treatment
- the actual or potential effectiveness of the treatment
- the acceptance of the treatment by medical experts.
You should be able to provide justification that your treatment is reasonably necessary. A medical referral alone is not sufficient to meet the ‘reasonably necessary’ benchmark.
Setting SMART goals
One of the principles of the Clinical Framework for the Delivery of Health Services is empowering the worker to manage their injury.
As an allied health practitioner working in the workers compensation scheme, you must identify Specific, Measurable, Achievable, Relevant and Timed (SMART) goals that have been developed in collaboration with and agreed to by the worker.
Goals created with the worker reflect their priorities and clearly outline their anticipated level of change. They are more meaningful to the worker and this increases their participation and encourages behavioural change.
Recovery goals should be Specific, Measurable, Achievable, Relevant and Timed (SMART):
Names the particular variable of interest (distance able to walk, hours at work, ability to concentrate on specific work task for 30 mins, able to drive children to local sports game, etc.).
Has a measurement unit (metres, hours, 0-10 scale).
Likely to be achieved given the diagnosis and prognosis for the person's injury and any environmental constraints.
Information must be relevant or important to the worker and other stakeholders.
Timeframe in which the goal is expected to be achieved.
Participation level goals are considered best practice in rehabilitation. These goals often describe a worker’s return to or progress towards an important life role.
Participation level goals are more likely to motivate the worker as they show how rehabilitation can help achieve outcomes relevant to them.
Impairment level goals are your goals related to the injury. They are objective and clinical, but not meaningful to the worker. For example, your impairment level goal might focus on an increase in range of motion.
It is expected that in the majority of cases, the goal(s) will remain the same throughout rehabilitation.
If you or the worker are having trouble moving beyond impairment level goals, you should ask the worker what they want this treatment to achieve.
Note: The insurer does not approve goals. Instead, they use these goals and other information to decide whether the services you propose are ‘reasonably necessary’.
The allied health recovery request
The allied health recovery request (AHRR) is the primary communication tool regarding the worker’s recovery and the provision of services. It facilitates communication between all members of the support team to ensure the worker receives appropriate, cost effective treatment with the best possible outcomes.
The AHRR allows you to:
- describe the impact of the injury on the worker in terms of reported and observed signs and symptoms, as well as their capacity to engage in their roles at work, home and in the community
- set SMART goals and empower the worker to be actively involved in their recovery
- outline an action plan, listing actions the worker and you are individually responsible for
- demonstrate the effectiveness of treatment using measurable outcomes
- request approval of treatment services, including equipment needs and case conferencing, using a rationale to support the services requested
- indicate the anticipated timeframe the recovery will take
- receive an insurer decision to your request.
You can request approval for up to eight treatment services on a single AHRR form. However, you should only request the number of sessions you believe the worker will need, and that you as the treatment provider can justify.
All sections of the AHRR should be completed to avoid any delays in processing and the provision of treatment.
You are required to submit an AHRR for any services requiring prior approval.
It is recommended you formulate the AHRR and submit it to the insurer prior to the completion of any currently approved (or where applicable sessions exempt from pre-approval) treatment sessions. This will assist with continuity of treatment.
You can request approval for up to a maximum of eight (8) consultations per allied health recovery request.
Refer to the workers compensation guidelines for further information.
Some services conducted by SIRA approved allied health practitioners are exempt from prior approval and do not require an allied health recovery request.
The type and number of services that may be provided depends on a number of factors, including how long it has been since the worker incurred their injury and whether they have received previous treatment for their injury.
Some exemptions from prior approval include:
- specific allied health treatment services
- case conferencing services that comply with the definition in the applicable Fees Order up to a maximum of two hours (refer to the 'Glossary' section for further information)
- reasonable incidental expenses (see 'Equipment provision' section below).
Non SIRA approved allied health practitioners should submit the AHRR after their first consultation with the worker.
Actively involving the worker in their treatment is an important part of effective rehabilitation.
Ensure the worker understands that they should be actively involved in their recovery – from setting goals and planning steps, to reviewing the progress of their recovery.
Complete the AHRR during a treatment session, or over consecutive treatment sessions, in consultation with the worker.
SIRA approved practitioners must provide their approval number on the AHRR. Once complete, you can send the AHRR to the insurer. Make sure you keep a record of when you sent the AHRR (e.g. email read receipts, fax transmission logs or a postal receipt).
Remember, after you complete and sign the AHRR you are responsible for its content.
If you are submitting the AHRR electronically you must be able to show that:
- you emailed the AHRR from the email address already provided to SIRA, or
- if the practice is emailing an AHRR on your behalf (and it contains your electronic signature) you have also provided written authorisation for the practice to do so.
It is inappropriate to complete the AHRR and insert the name and provider number of the practice principal or another allied health practitioner.
Allied health practitioners who are dual SIRA approved and concurrently delivering services under more than one discipline to a worker must provide one AHRR per discipline.
Where a multidisciplinary team is delivering services to a worker, a lead allied health practitioner may develop the goal with the worker, however, each practitioner must then complete their own AHRR using that goal, with consideration given to whether the provision of treatment concurrently by multiple disciplines is appropriate and can be clinically justified.
You can only bill the insurer once per claim for the initial allied health recovery request. Use the code OAS003 at the specified amount shown in your discipline specific Fees Order.
The Allied health recovery request (AHRR) – instructions for completion provides practitioners with step-by-step guidance on completing the AHRR.
The Allied health recovery request (AHRR) – instructions for completion provides practitioners with step-by-step guidance on completing the AHRR.
When an AHRR is submitted to the insurer, they must determine liability within 21 calendar days.
Concurrent treatment sessions
It is difficult to effectively monitor and measure the outcomes of each treatment when similar treatments are delivered concurrently. So we encourage practitioners to consider the principles of the Clinical Framework for the Delivery of Health Services during the initial discussion or consultation with the worker and question whether duplication of treatment for the same injury from separate practitioners can be justified.
When a worker is referred from one allied health practitioner to another for management of the same injury area, we recommend insurers fund up to two concurrent sessions for the referring practitioner to facilitate the transition of management (if required). Practitioners are expected to collaborate in these instances to ensure the effective continuation of the worker’s rehabilitation.
It is recommended the allied health practitioner receiving a referral ensure they inform the nominated treating doctor (if the referral was not received from the doctor), that they have been requested to treat the worker, as the doctor is responsible for coordinating the worker’s rehabilitation and clinical management.
Work is treatment
As we outlined in the Introduction, research shows that recovering at work after a work-related injury or illness can be beneficial to a worker’s recovery. Evidence shows:
- good work is therapeutic and promotes recovery4, 5
- safe work is good for you physically, socially and financially6, 7
- time off work is often not medically necessary and can delay recovery7
- the longer a worker is off work the less likely they are to ever return8
Supporting a worker to stay at work in some capacity or recover at work provides the best chance of a positive outcome following their injury. It’s also better for the workplace.
As an allied health practitioner, you should be prepared to discuss recovery at/return to work options with the worker and support team.
Allied health practitioners and the workplace
In the NSW workers compensation scheme, allied health practitioners do not have approval to enter a workplace to provide treatment services for a worker. This does not apply to on-site treatment facilities funded by an employer as part of their general health, safety and wellness staff initiatives.
In the exceptional circumstance where proposed treatment can only be provided in the workplace, you must seek pre-approval from the insurer and the employer to deliver the service in the work environment.
You should only request this where it is essential the treatment be provided in the work environment, based on the needs of the worker and the type of treatment proposed. For example, psychological treatment using systematic desensitisation. Treatment inside the workplace can only proceed where all parties have consented to the arrangement.
Mediation is not a treatment service and therefore cannot be provided by a treating allied health practitioner in the NSW workers compensation scheme.
Equipment provision
Reasonable incidental expenses for items the worker takes with them for independent use (e.g. strapping tape, TheraBand, disposable electrodes, exercise putty, walking sticks, relaxation CDs and self-help books) are payable in addition to the consultation fee.
This does not apply to consumables or exercise handouts used during a consultation (e.g. anti-inflammatory creams, ultrasound gel, acupuncture needles, tissues and so on). These items are considered a business expense.
Where you recommend equipment for the worker, insurer approval must be obtained prior to purchasing or hiring the equipment (unless pre-approval exemptions apply). Without prior approval, the insurer is not liable for the cost of the equipment.
SIRA approved practitioners may bill up to $110 per claim for incidental expenses and equipment provision, without obtaining prior approval from the insurer.
A description of the item must appear on the invoice forwarded to the insurer.
Any request for equipment with a total cost above $110 requires prior approval from the insurer.
Non SIRA approved practitioners require prior approval for all incidental expenses and equipment provision.
If through discussions with the worker, you identify that equipment at the workplace may assist their recovery at/return to work, please advise the insurer. This equipment may be arranged by the insurer with the assistance of other members of the support team at the workplace.
To support therapeutic and recovery at/return to work goals, the worker may require an allied health practitioner to assess and recommend practical aids/disability equipment/home modifications and domestic assistance.
Gym/pool based programs
SIRA does not generally support the use of pool or gym programs for work related injuries.
In many cases, activity can be prescribed so that it can be performed in the worker’s usual settings without the need to introduce an alternate setting such as the gymnasium or pool. This supports the worker’s progression towards self-management, rather than developing reliance on equipment that is not available at work or home, and/or on the attending practitioner.
In exceptional circumstances, insurers may consider funding treatment at a gymnasium or pool. These programs should be tailored to the worker’s compensable injury and specific rehabilitation needs.
Generally, pool based treatment is used to aid transition between non-weight-bearing and land-based treatments and therefore is not considered an ongoing treatment alternative. It is expected that gym/pool programs will not be a standard duration (for example one month), but rather will be requested as a defined number of sessions on the AHRR, based on the intended outcome of the program.
Where a gym/pool based program is developed, it should be formulated so the worker can complete it independently. The program should form part of a self-managed rehabilitation plan and facilitate recovery at/return to work. It is expected that your input will be limited to the set-up of the gym/pool program, periodic review and evaluation.
Note: Water based programs will not be approved where the worker has already returned to work or achieved capacity to work.
Treating workers with severe injury
Parts of this guide may not apply to practitioners delivering specialised services to workers who have been severely injured at work.
The NSW workers compensation system uses the following specific criteria regarding eligibility for treatment for workers with severe injury. Severe injury means one or more of the following diagnoses (and associated criteria) are met:
Acute traumatic lesion of the neural elements in the spinal canal (spinal cord and cauda equina) resulting in permanent sensory deficit, motor deficit or bladder/bowel dysfunction as a result of the work-related injury.
Based on evidence of a significant brain injury which results in permanent impairments of cognitive, physical and/or psychosocial functions.
A defined period of post traumatic amnesia plus a Functional Independence Measure (FIM) at five or less, or two points less than the age appropriate norm (or equivalent where other assessment tools are used) is required.
- multiple amputations (or equivalent loss of function) of the upper and/or lower extremities or single amputations (or equivalent loss of function) involving forequarter amputation or shoulder disarticulation, hindquarter amputation, hip disarticulation or "short" trans femoral amputation involving the loss of 65% or more of the length of the femur.
Full thickness burns greater than 40 per cent of the total body surface area or full thickness burns to the hands, face or genital area, or inhalation burns causing long term respiratory impairment, plus a FIM score at five or less, or two points less than the age norm (or equivalent where other assessment tools are used).
Permanent traumatic blindness, based on the legal definition of blindness.
It is expected that only a very small number of practitioners will be providing specialised services to workers who meet the definition of severe injury.
We know treatment needs may differ significantly for a worker with a severe injury. While return to work is still a focus, it may not be possible for all workers with a severe injury.
In this case the support team will focus on other meaningful activities to improve the worker’s independence and participation in their home and community. Services may be coordinated by a case manager external to the insurer.
The insurer must provide prior approval for all treatment services. It is recommended that you contact the insurer to:
- confirm you are treating a worker with a recognised severe injury
- discuss the appropriate way of requesting services.
Use of the AHRR is optional for the request of services for workers with severe injury.
SIRA approved practitioners delivering specialised services to workers with severe injury are allowed greater flexibility when tailoring treatment. This may include the following:
- services provided are exempt from the NSW Workers Compensation Fees Orders
- practitioners may bill for their time to undertake comprehensive assessment and/or treatment services, where required
- practitioners are able to provide multiple services on the same day where required, for example treatment of the worker and education of family/carers
- physical treatment practitioners may deliver treatment concurrently with other physical treatment practitioners, where appropriate.
This flexibility aims to meet the unique needs of a worker with a severe injury and to remunerate the practitioner appropriately for their services.
Non SIRA approved practitioners delivering specialised services to workers with severe injury are to discuss their fees with the insurer and agree upon an appropriate charge at the time of requesting approval to deliver services (except for massage therapists who have their own Fees Order).
Telehealth
Allied health practitioners can bill for telehealth consultations where they meet the requirements in Part 2 of the Guidelines for the Provision of Relevant Services (Health and Related Services).
Telehealth services must be provided in combination with in-person services unless the services are:
- allied health mental health treatment services, or
- pre-approved by the insurer managing the injured person’s claim for delivery exclusively by telehealth.
Telehealth services must be provided by videoconference unless it is unavailable. Email, SMS, or an app may only be used in conjunction with the delivery of telehealth via videoconference
The use of telehealth for consultations must comply with the requirements in 2.5 of the Guidelines for the Provision of Relevant Services (Health and Related Services), including that it has been consented to by the worker.
Telehealth services are billed under a different payment code to a face to face consultation. Refer to the applicable fees order for further information.
Fees
Treatment delivered by SIRA approved practitioners is defined and governed by the relevant Workers Compensation Fees Orders and the Guidelines for the Provision of Relevant Services (Health and Related Services).
Under Part 5 of the Guidelines for the Provision of Relevant Services (Health and Related Services) allied health practitioners must not:
- request pre-payment of fees for reports and services from the insurer
- directly bill relevant services to an injured worker who has already lodged a claim
- bill an amount that is above the maximum amount fixed in the SIRA fees order
- charge the injured person any additional or gap fee
- charge a fee for cancellation or non-attendance by an injured worker for treatment services.
If you attempt to charge either the insurer or worker more than the maximum fee, you risk SIRA revoking your approval, or a direction being given under section 26D of the SICG Act. Current Workers Compensation Fees Orders are available on our website.
Except for massage therapy, SIRA has not set maximum fees for treatment delivered by non-SIRA approved allied health practitioners.
For services delivered by a non-SIRA approved allied health practitioner that are similar in nature to that of a SIRA approved practitioner (e.g. hand therapy by an occupational therapist), it is recommended the relevant SIRA fees order be used as a guide for the cost of services.
You (other than massage therapists) must discuss fees with the insurer and agree upon an appropriate charge at the time of requesting approval. The fee should be similar to the amount customarily paid within the community for that type of treatment or service (except for massage therapists who have their own Fees Order).
When the insurer notifies you of the approval for treatment or services, they should specify the costs approved.
Under Part 5 of the Guidelines for the Provision of Relevant Services (Health and Related Services) allied health practitioners must not:
- request pre-payment of fees for reports and services from the insurer
- directly bill relevant services to an injured worker who has already lodged a claim
- bill an amount that is above the maximum amount fixed in the SIRA fees order
- charge the injured person any additional or gap fee
- charge a fee for cancellation or non-attendance by an injured worker for treatment services.
Massage therapists should be aware that if you attempt to charge either the insurer or worker more than the maximum fee, you risk a direction being given under section 26D of the SICG Act. Current Workers Compensation Fees Orders are available on our website.
When invoicing, the service provider number for interstate practitioners is INT0000. The payment classification code is the one relevant to your professional discipline.
Any accredited exercise physiology, chiropractic, counselling, osteopathy, massage therapy, physiotherapy or psychological treatment services provided to a NSW worker in a state or territory other than NSW, must be paid in accordance with the fee that would apply to the workers compensation jurisdiction of the state/territory of service, up to the maximum fee specified in the schedule of the relevant NSW Fees Order.
Invoicing
Part 6 of the Guidelines for the Provision of Relevant Services (Health and Related Services) requires that allied health practitioners must provide itemised invoices before payment can be made by the insurer; and that invoices for relevant services rendered must be submitted within 30 calendar days of the service provided and include:
- the injured worker’s first and last name, and claim number
- payee name, address, telephone number and email address
- payee Australian Business Number (ABN)
- name of the relevant service provider who delivered the relevant service
- in the case of allied health services, the following provider numbers:
- the provider’s SIRA approval number (where applicable), and
- the provider’s AHPRA number/professional association accreditation/membership number
- in the case of allied health services provided interstate by a service provider who doesn’t have a SIRA approval number, the service provider number INT0000 must be included on the invoice instead
- in the case of allied health services provided to exempt workers, by a service provider who doesn’t have a SIRA approval number, the service provider number EXT0000 must be included on the invoice instead.
- relevant SIRA payment classification code (where applicable)
- service cost for each SIRA payment classification code (if applicable)
- date of service
- date of invoice (must be on the day of or after last date of service listed on the invoice).
Cancellation or failure to attend
No fees are payable for worker cancellation or failure to attend scheduled sessions.
You are encouraged to schedule treatment sessions outside the worker’s work commitments in order to maximise attendance rates.
No pre-payment for planned services
You must not request pre-payment of fees for reports and services from the insurer. Insurers are not authorised to pay allied health practitioners in advance of services being provided, even where approval has been given to provide those services. This includes report writing.
When worker circumstances change
Circumstances concerning worker eligibility for medical and related expenses may change.
Treatment may have been approved but then, due to circumstances changing with the claim status, treatment funding is no longer available. This may occur because:
- the worker’s claim has been disputed, commuted or settled
- information is obtained by the insurer and they have determined treatment is no longer reasonably necessary
- time limit thresholds have been met.
You should clarify eligibility prior to your initial consultation with the worker, resumption of treatment, or where you believe other circumstances have changed which may impact the worker’s eligibility to medical and related expenses.
Independent consultants
Independent consultants listed on SIRA’s website are able to provide an independent peer review of allied health treatment and the management of individual cases.
Independent consultants may:
- complete a biopsychosocial assessment of the worker with consideration given to their diagnosis and prognosis
- determine whether further treatment is reasonably necessary
- advise the treating practitioner, insurer and worker on the need for further treatment
- work with the treating practitioner to decide future treatment content, the duration that will achieve the best outcomes for the worker and increase the worker’s capacity for employment
- educate allied health practitioners about the NSW workers compensation scheme.
They do not:
- determine causation or liability
- undertake a functional capacity evaluation or any formal assessment of work capacity for the insurer for the purposes of assessing work capacity.
Allied health practitioners must participate in peer reviews of the injured person's injury, treatment, and recovery,
Who can be an independent consultant?
SIRA approval is required to be an independent consultant. The practitioner must meet the following criteria:
- is an allied health practitioner registered with AHPRA. They could be either be:
- a physiotherapist, chiropractor or osteopath for the review of physical treatment, or
- a psychologist for the review of psychological treatment.
- is experienced in delivering health services within the NSW workers compensation scheme
- has satisfied the SIRA selection criteria and agreed to the conditions of approval
Independent consultants are approved for three-years (with an option for SIRA to extend this to a maximum of five years) and are listed on our website as an independent consultant.
Referral to an independent consultant
A referral for an independent consultant review should occur early in the recovery process in order to achieve the best outcome for the worker.
Any member of the support team may recommend a referral to an independent consultant. The insurer will approve the referral and complete the referral form with the information provided from any third party. A standard referral template should be used and is available on our website.
The independent consultant should be (where possible) of the same discipline as the allied health practitioner managing the worker.
A referral may be initiated in the following ways:
The insurer should consider a referral to an independent consultant where an allied health practitioner requests treatment continues beyond 16 sessions, or if, after discussion with the treating allied health practitioner, there is concern about:
- the treatment duration, frequency and/or whether treatment is reasonably necessary
- treatment that has continued for an extended period without any improvement in functional outcomes, particularly in relation to a worker’s capacity
- the treatment approach most likely to achieve positive work outcomes for the worker
- barriers to recovery at work and/or psychosocial risk factors for delayed recovery and work loss.
The insurer should confirm the appropriateness of the referral to an independent consultant using their own internal resources (for example injury management advisor, team leader). They should also ensure that there is no conflict of interest between the independent consultant and allied health practitioner.
As an allied health practitioner, you are encouraged to request involvement of an independent consultant where barriers to recovery, progress, return to work or active participation are evident, and you consider that an independent opinion and/or expert advice is likely to be beneficial in the management of the worker’s injury.
SIRA supports the proactive involvement of an independent consultant in these cases in order to achieve the best outcome for the worker.
Contact the insurer by telephone or note your request and rationale in the space provided on the AHRR.
Other members of the support team, such as the employer, doctor, workplace rehabilitation provider or worker, can request an independent consultant review if recovery progress has been delayed, or if guidance regarding treatment management options is required.
Approving and arranging an independent consultant referral
Before they approve a referral to an independent consultant, the insurer will make direct contact with the allied health practitioner in order to discuss worker treatment, progress and the referral.
Any referral to an independent consultant is to be arranged by the insurer not a third party such as a medico-legal company.
Once the referral is approved the insurer is required to:
- select an independent consultant from those listed on the SIRA website (from the same discipline as the treating allied health practitioner if possible)
- complete the referral form, attach all relevant information and email it to the independent consultant
- approve the stage of review (one, two or three) after discussion with the independent consultant
- inform the treating allied health practitioner, worker and nominated treating doctor of the referral and its purpose.
It is recommended the insurer consider approval for a limited number of treatment sessions while the referral and review are undertaken, as halting treatment may lead to additional barriers to progress.
Independent consultant reviews
An independent consultant review can take three forms:
This involves a review of the AHRR(s) and/or other relevant documentation, to help the insurer determine reasonably necessary treatment services or equipment prescription.
This is only to occur where the specialised skills of an independent consultant are required. The independent consultant is not to replace the role of the insurer’s injury management advisor.
This involves the consideration of all AHRR(s) and other relevant documentation, as well as a verbal discussion with the treating allied health practitioner.
The discussion with the treating practitioner is likely to include current treatment outcomes, proposed treatment and intervention to build the worker’s capacity for employment.
If after the review of the referral information, the independent consultant determines an assessment of the worker is required for an effective review, they will ask the insurer to advise the worker of what is involved and arrange an appointment.
Discussion with the treating practitioner is likely to include current treatment outcomes, proposed future treatment, and intervention to build the worker’s capacity for employment.
In stage two and three reviews, discussion with the treating allied health practitioner is an important part of the independent consultant review process.
Treating practitioners must participate in a verbal discussion with the independent consultant, unless extenuating circumstances prevent them from doing so (for example hearing impairment). In this situation, alternative communication means are to be used.
The independent consultant review may contain any discussion regarding the assessment, treatment and services relating to the workers compensation claim.
Discussions should be arranged within business hours unless another time is mutually agreed. Responses to contact made by the independent consultant should be provided by the allied health practitioner within three working days, unless reasonable circumstances prevent contact within this time frame. A mutually convenient time for discussions must be scheduled within two working weeks of the independent consultant’s initial contact.
Non participation in independent consultant reviews by practitioners are required to be reported to SIRA by independent consultants and may impact on a practitioner’s SIRA approval and/or application for re-approval.
SIRA approved allied health practitioners must participate in a review when they are contacted by an independent consultant. SIRA may suspend or revoke its approval of an allied health practitioner if the practitioner fails to cooperate with the independent consultant. Refer to the Guideline for approval of treating allied health practitioners on our website for more information.
Non SIRA approved allied health practitioners are asked to participate fully in independent consultant reviews when contacted.
Non SIRA approved allied health practitioners must participate in independent consultant reviews when contacted.
Once the review is complete, the independent consultant will provide a report with recommendations to the support team and worker (unless release of the report would pose a serious threat to the life or health of the worker or any other person).
They should provide their report within 10 working days of the review, unless prior arrangements with a different timeframe have been made with the insurer.
The insurer’s decision about funding future treatment will take into account the recommendations of the independent consultant, as well as other information available at the time. Independent consultant recommendations are not binding but influential in guiding decisions about future treatment.
The insurer is responsible for implementing and monitoring the recommendations in a timely manner.
Services provided by an independent consultant are paid for by the insurer and are charged as a cost to the claim. The Workplace Injury Management and Workers Compensation (Independent Consultant) Fees Order applies. Learn more on our website.
Please note, no fee is payable to treating allied health practitioners for time spent liaising with an independent consultant.

Further information
More information about workers compensation claims, insurance and work health safety matters is available on our website or you can call us on 13 10 50.
Glossary
The AHRR is the primary communication tool between allied health practitioners and the insurer when discussing the worker’s recovery and the provision of services.
It facilitates effective communication between all members of the support team and ensures the worker receives appropriate, cost effective treatment with the best possible outcomes.
“Case conference” means face-to-face meeting, video conference or teleconference with any or all of the following:
- the worker (including a support person, if requested by the worker)
- employer
- workplace rehabilitation practitioner
- insurer; and/or
- other treatment practitioner/s delivering services to the worker (including the nominated treating doctor)
The following are not considered a case conference and are not to be charged as such:
- discussions with the worker only (and a support person, if requested by the worker)
- discussions with Independent Consultants
- discussions between treating doctors and counsellors relating to treatment.
Case conferences must:
- seek to clarify the worker’s capacity for work, barriers to return to work, and strategies to overcome these barriers
- be an open forum to ensure parties are aligned with respect to expectations and direction of the worker’s recovery at work or return to suitable employment.
Practitioner file notes of case conferences are to be documented in the allied health practitioner’s records indicating the person(s) spoken to, details of discussions, duration of the discussion and outcomes. This information may be required for invoicing or auditing purposes.
SIRA approved allied health practitioners
Prior approval is not required for up to two hours of case conferencing per claim. It is to be billed according to the relevant Fees Order.
Non SIRA approved allied health practitioners
Prior approval is required for case conferencing per claim. It should be billed using the relevant NSW workers compensation Fees Order as a guide to the appropriate fee.
A dispute happens when the insurer decides, based on available evidence, that a person does not meet the legal requirements to be entitled to workers compensation benefits.
An insurer may dispute a claim for many reasons, including, but not limited to:
- liability of the claim (insurer disputes all or part liability for a claim)
- injury management (suitable employment or medical treatment)
- permanent impairment (level of permanent impairment).
As stated in s59A of the Workers Compensation Act 1987, workers may have an eligibility time limit for insurer payment of medical and related expenses.
Exempt workers and existing claims have different medical and related expense time limits.
Upon referral, contact the insurer to confirm the:
- status of the worker’s claim
- worker is eligible for payment of medical and related expenses
- insurer agrees treatment is reasonably necessary.
When treatment resumes for the same injury more than three months after the last session of treatment it is considered to be a new episode of care.
The Workers Compensation Legislation Amendment Act 2012 changed the workers compensation laws. The 2012 amendments do not apply to police officers, paramedics or fire fighters – these are exempt workers.
For further information please review the Guidelines for claiming workers compensation.
Injury management is the process that comprises activities and procedures that are undertaken or established for the purpose of achieving a timely, safe and durable recovery at/return to work for workers following a work-related injury or illness.
An injury management plan must be developed by the insurer in consultation with the employer (except when the insurer is a self-insurer), nominated treating doctor and the worker. It is used to coordinate and manage the treatment, rehabilitation and training (where appropriate) of the worker.
A plan must be established for a work-related injury if the worker is unable to work for a continuous period of more than seven days.
Refers to the three types of insurers in the NSW workers compensation system:
- The Workers Compensation Nominal Insurer (Nominal Insurer). icare acts for the Nominal Insurer.
- Self-insurers
- Specialised insurers.
As an allied health practitioner, you will work with a specific insurer case manager for each workers compensation claim.
See our website for more information.
Non SIRA approved allied health practitioners include all other allied health practitioner disciplines not listed as SIRA approved practitioners.
See our website for more information.
The insurer may make provisional payments before it determines liability to cover:
- up to 12 weeks of payments for loss of income
- up to $7,500 for reasonably necessary medical treatment.
Provisional payments do not apply in some situations, for example, for rural fire fighters, emergency service and rescue association volunteers.
The insurer may have ‘reasonable excuse’ not to start provisional payments, for example:
- there is insufficient medical information
- the injured person is unlikely to be a worker
- the insurer is unable to contact the worker
- the worker refuses access to information
- the injury is not work related
- there is no requirement for weekly payments
- the injury is not notified within two months.
A timely, safe and durable return to paid employment for which the person is suited, having particular regard to their capacity, pre-injury employment, age, education, skills and work experience.
A statement of goals and objectives (and services required to achieve them) for a worker undergoing recovery at work. It should clearly outline the worker’s capacity for work including hours, supervision requirements, treatment times and review dates.
The plan is usually developed by the employer or workplace rehabilitation provider (where involved) and should be done so in consultation with the worker. It should be regularly monitored against the worker’s progress.
SIRA approved allied health practitioners include:
- physiotherapists, chiropractors and osteopaths
- psychologists, counsellors
- accredited exercise physiologists.
For more information regarding SIRA approved allied health practitioners, visit our website.
The Workers Compensation (Bush Fire, Emergency and Rescue Services) Act 1987 provides compensation coverage for rural fire fighters, emergency service and rescue association volunteers in the event they are injured in the course of authorised activities.
See www.legislation.nsw.gov.au for more information.
A worker who has sustained a work-related injury or illness and is entitled to compensation under NSW workers compensation legislation.
In this document ‘worker’ also includes exempt workers, volunteers and emergency rescue workers under the Workers Compensation (Bush Fire, Emergency and Rescue Services) Act 1987 unless otherwise stated.
Frequently asked questions
Any items used during the treatment session such as needles, strapping tape, oils, creams/gels, exercise handouts and so on, are considered a business expense and the cost is included in the consultation fee. No additional fee is payable for these items.
For SIRA approved allied health practitioners
SIRA approved allied health practitioners can bill up to $110 per claim for incidental expenses without insurer's prior approval.
For non-SIRA approved allied health practitioners
Non-SIRA approved allied health practitioners are required to seek prior approval for all incidental expenses.
If the treatment is delivered on an individual basis, the standard consultation rate listed in the relevant Fees Order should be used, regardless of the type of treatment delivered during the consultation.
The following exceptions apply (as per the definitions stated in the relevant Fees Order):
- the treatment is for three or more entirely compensable injuries or conditions
- the treatment is for major hand injury (modified Hand Injury Severity Score >100) where assessment and treatment is provided by an Australian Hand Therapy association Accredited Hand Therapist, or
- extensive burns, or
- you are treating a worker with a severe injury.
Insurers expect the allied health practitioner to communicate via the AHRR.
If you receive a request from the insurer for a report, you will receive pre-approval to bill for a maximum of one hour.
If you do not think you can answer the questions posed by the insurer adequately in this time, you should contact the referrer and inform them you will be unable to address all issues/questions raised. Ask them to reconsider the questions they have asked you, to enable you to complete the report within the maximum one hour period.
The insurer will not pay for a report that has not been requested.
There is no fee payable for non-attendance. Allied health practitioners should implement scheduling systems which maximise worker attendance rates. This may mean scheduling an appointment outside their work hours.
No. You cannot bill the worker for non-attendance or a gap fee.
You should discuss the issue of non-attendance with the worker and explain the impact on their likely progression and recovery.
You may need to remind the worker that continued non-attendance will be discussed with the insurer and their employer.
Travel costs require pre-approval from the insurer.
Travel costs may be approved where the most appropriate clinical management of the worker requires the allied health practitioner to travel away from their commercial place of business . This usually only applies to workers with a severe injury (as per the definition outlined in the Fees Orders).
Travel costs cannot be charged:
- where the allied health practitioner provides services to facilities such as a private hospital
- where a practitioner does not have (or is employed by a business that does not have) a commercial place of business for the delivery of treatment services (e.g. mobile practice).
Where multiple clients are being treated in the same visit to a facility or in the same geographical area on the same day, the reasonable travel charge must be divided evenly between those workers.
This is correct. EFT is now the only payment method from insurers to third party service providers.
Payment will not be made for the delivery of more than one consultation with the worker each day. However, if you are providing treatment to a worker with a severe injury (as per the definition in the Fees Orders) this rule does not apply.
SIRA does not generally support the use of pool or gym programs for work related injuries.
In many cases activity can be prescribed so that it can be performed in the worker’s usual settings, without the need to introduce an alternate setting such as a gymnasium. This also supports early progression towards self-management, rather than developing reliance on equipment that is not available at work or home, and/or on the attending allied health practitioner.
Water-based programs will not be approved where the worker has already returned to work.
In exceptional circumstances when approval is given for treatment to be provided at an external facility such as a gymnasium or pool, the facility (and not the allied health practitioner) is to invoice the insurer directly under code OTT007. Where this is not possible, the allied health practitioner must clearly state the name, location and charge cost price of the facility on their invoice and attach a copy of the facility’s invoice to their account.
External facility fees only apply to the cost of the worker’s entry. An entry fee will not be paid where the facility is owned or operated by the allied health practitioner or the allied health practitioner contracts their services to the facility. Fees payable for the entry of the allied health practitioner are a business cost and cannot be charged to the insurer.
References
- Australasian Faculty of Occupational and Environmental Medicine and The Royal Australasian College of Physicians. (2011.) 'Australian Consensus Statement on the Health Benefits of Work.' A Position Statement.
- Waddell G, Burton A, Bartys S. (2004.) Concepts of rehabilitation for the management of common health problems - evidence base. Project Report. Department of Work and Pensions, H M Government, The Stationery Office, London.
- Foreman P, Murphy G and Swerissen H. (2006.) Barriers and facilitators to return to work: A Literature Review. Australian Institute for Primary Care, La Trobe University, Melbourne.
- Cheng and Hung. (2007.) Randomized Controlled Trial of Workplace-based Rehabilitation for Work-related Rotator Cuff Disorder. J Occup Rehab 17:487-503.
- The Royal Australasian College of Physicians and the Australasian Faculty of Occupational and Environmental Medicine. (2013.) What is good work? A Position Statement.
- Waddell G and Burton K. (2006.) Is work good for your health and wellbeing? Department of Work and Pensions, H M Government, The Stationery Office, London.
- Australasian Faculty of Occupational and Environmental Medicine and the Royal Australasian College of Physicians. (2011.) Australian Consensus Statement on the Health Benefits of Work. A Position Statement.
- Johnson D, Fry T. (2002.) Factors Affecting Return to Work after Injury: A study for the Victorian WorkCover Authority. Melbourne Institute of Applied Economic and Social Research, The University of Melbourne.
Acknowledgements
This guide was developed by SIRA to facilitate communication between allied health practitioners, insurers and other members of the worker's support team.
It was developed in conjunction with the Allied Health Practitioner Management Framework Review working party. The working party was made up of representatives from each workers compensation insurer, the Nominal Insurer icare, Lifetime Care, Dust Diseases Care, Motor Accidents Insurance Regulation, the Australian Physiotherapy Association, the Australian Psychological Society, Exercise & Sports Science Australia, independent consultants and Workers Compensation Regulation. SIRA would like to thank the working party for their input during this process.
This guide was updated in December 2023.
Updated 21 July 2025