NSW workers compensation guidelines for the evaluation of permanent impairment
These guidelines explain permanent impairment assessment in the NSW workers compensation system. This is the fourth edition of these guidelines, reissued 1 March 2021.
Download a PDF of this document in full.
Click here to read the foreword
The State Insurance Regulatory Authority has reissued the 4th edition of the NSW workers compensation guidelines for the evaluation of permanent impairment (catalogue no. WC00970) (the Guidelines) for assessing the degree of permanent impairment arising from an injury or disease within the context of workers’ compensation. When a person sustains a permanent impairment, trained medical assessors must use the Guidelines to ensure an objective, fair and consistent method of evaluating the degree of permanent impairment.
The reissued Guidelines have been made to include some minor changes including changes consequent to the enactment of the Personal Injury Commission Act 2020 (PIC Act). No changes are made to the provisions in these guidelines relating to the evaluation of permanent impairment as developed in consultation with the medical Colleges under s 377(2) of the Workplace Injury Management and Workers Compensation Act 1998 and as set out in cl 13 of the Guidelines.
The Guidelines are based on a template that was developed through a national process facilitated by Safe Work Australia. They were initially developed for use in the NSW system and incorporate numerous improvements identified by the then WorkCover NSW Whole Person Impairment Coordinating Committee over 13 years of continuous use. Members of this committee and of the South Australia Permanent Impairment Committee (see list in Appendix 2) dedicated many hours to thoughtfully reviewing and improving the Guidelines. This work is acknowledged and greatly appreciated.
The methodology in the Guidelines is largely based on the American Medical Association’s Guides to the Evaluation of Permanent Impairment, 5th Edition (AMA5). The AMA guides are the most authoritative and widely used in evaluating permanent impairment around the world. Australian medical specialists representing Australian medical associations and colleges have extensively reviewed AMA5 to ensure it aligns with clinical practice in Australia.
The Guidelines consist of an introductory chapter followed by chapters dedicated to each body system.
The Introduction is divided into three parts. The first outlines the background and development of the Guidelines, including reference to the relevant legislative instrument that gives effect to the Guidelines. The second covers general assessment principles for medical practitioners applying the Guidelines in assessing permanent impairment resulting from work-related injury or disease. The third addresses administrative issues relating to the use of the Guidelines.
As the template national guideline has been progressively adapted from the NSW Guideline and is to be adopted by other jurisdictions, some aspects have been necessarily modified and generalised. Some provisions may differ between different jurisdictions. For further information, please see the Comparison of Workers’ Compensation Arrangements in Australia and New Zealand report, which is available on Safe Work Australia’s website.
Publications such as this only remain useful to the extent that they meet the needs of users and those who sustain a permanent impairment. It is, therefore, important that the protocols set out in the Guidelines are applied consistently and methodically. Any difficulties or anomalies need to be addressed through modification of the publication and not by idiosyncratic reinterpretation of any part. All queries on the Guidelines or suggestions for improvement should be addressed to SIRA at [email protected].
Chapters
Chapters
- Introduction
- Upper extremity
- Lower extremity
- The spine
- Nervous system
- Ear, nose, throat and related structures
- Urinary and reproductive systems
- Respiratory system
- Hearing
- The visual system
- Psychiatric and psychological disorders
- Haematopoietic system
- The endocrine system
- The skin
- Cardiovascular system
- Digestive system
- Evaluation of permanent impairment arising from chronic pain
- Appendix 1. Key definitions
- Appendix 2. Working groups on permanent impairment
4. The spine
AMA5 Chapter 15 (p 373) applies to the assessment of permanent impairment of the spine, subject to the modifications set out below. Before undertaking an impairment assessment, users of the Guidelines must be familiar with:
- the Introduction in the Guidelines
- chapters 1 and 2 of AMA5
- the appropriate chapter(s) of the Guidelines for the body system they are assessing.
- the appropriate chapter(s) of AMA5 for the body system they are assessing.
- The Guidelines take precedence over AMA5.
Introduction
4.1 The spine is discussed in Chapter 15 of AMA5 (pp 373–431). That chapter presents two methods of assessment, the diagnosis-related estimates method and the range of motion method. Evaluation of impairment of the spine is only to be done using diagnosis-related estimates (DREs).
4.2 The DRE method relies especially on evidence of neurological deficits and less common, adverse structural changes, such as fractures and dislocations. Using this method, DREs are differentiated according to clinical findings that can be verified by standard medical procedures.
4.3 The assessment of spinal impairment is made when the person’s condition has stabilised and has reached maximum medical improvement. This is considered to occur when the worker’s condition is well stabilised and unlikely to change substantially in the next year, with or without medical treatment. If surgery has been performed, the outcome of the surgery as well as structural inclusions must be taken into consideration when making the assessment.
Assessment of the spine
4.4 The assessment should include a comprehensive, accurate history, a review of all pertinent records available at the assessment, a comprehensive description of the individual’s current symptoms and their relationship to activities of daily living (ADL); a careful and thorough physical examination; and all findings of relevant laboratory, imaging, diagnostic and ancillary tests available at the assessment. Imaging findings that are used to support the impairment rating should be concordant with symptoms and findings on examination. The assessor should record whether diagnostic tests and radiographs were seen or whether they relied solely on reports.
4.5 The DRE model for assessment of spinal impairment should be used. The range of motion model (AMA5 sections 15.8–15.13 inclusive, pp 398–427) should not be used.
4.6 If a person has spinal cord or cauda equina damage, including bowel, bladder and/or sexual dysfunction, he or she is assessed according to the method described in AMA5 Section 15.7 and AMA5 Table 15.6 (a)–(g) (pp 395–98).
4.7 If an assessor is unable to distinguish between two DRE categories, then the higher of those two categories should apply. The reasons for the inability to differentiate should be noted in the assessor’s report.
4.8 Possible influence of future treatment should not form part of the impairment assessment. The assessment should be made on the basis of the person’s status at the time of interview and examination, if the assessor is convinced that the condition is stable and permanent. Likewise, the possibility of subsequent deterioration, as a consequence of the underlying condition, should not be factored into the impairment evaluation. Commentary can be made regarding the possible influence, potential or requirements for further treatment, but this does not affect the assessment of the individual at the time of impairment evaluation.
4.9 All spinal impairments are to be expressed as a percentage of WPI.
4.10 AMA5 Section 15.1a (pp 374–77) is a valuable summary of history and physical examination, and should be thoroughly familiar to all assessors.
4.11 The assessor should include in the report a description of how the impairment rating was calculated, with reference to the relevant tables and figures used.
4.12 The optimal method to measure the percentage compression of a vertebral body is a well-centred plain X-ray. Assessors should state the method they have used. The loss of vertebral height should be measured at the most compressed part and must be documented in the impairment evaluation report. The estimated normal height of the compressed vertebra should be determined, where possible, by averaging the heights of the two adjacent (unaffected and normal) vertebrae.
Specific interpretation of AMA5
4.13 The range-of-motion (ROM) method is not used, hence any reference to this is omitted (includingAMA5 Table 15-7, p 404).
4.14 Motion segment integrity alteration can be either increased translational or angular motion, or decreased motion resulting from developmental changes, fusion, fracture healing, healed infection or surgical arthrodesis. Motion of the individual spine segments cannot be determined by a physical examination, but is evaluated with flexion and extension radiography.
4.15 The assessment of altered motion segment integrity is to be based upon a report of trauma resulting in an injury, and not on developmental or degenerative changes.
4.16 When routine imaging is normal and severe trauma is absent, motion segment disturbance is rare. Thus, flexion and extension imaging is indicated only when a history of trauma or other imaging leads the physician to suspect alteration of motion segment integrity.
DRE definitions of clinical findings
4.17 The preferred method for recording ROM is as a fraction or percentage of the range or loss of the range. For example, either ‘cervical movement was one half (or 50%) of the normal range of motion’ or ‘there was a loss of one half (or 50%) of the normal range of movement of the cervical spine’.
4.18 DRE II is a clinical diagnosis based upon the features of the history of the injury and clinical features. Clinical features which are consistent with DRE II and which are present at the time of assessment include radicular symptoms in the absence of clinical signs (that is, non-verifiable radicular complaints), muscle guarding or spasm, or asymmetric loss of range of movement. Localised (not generalised) tenderness may be present. In the lumbar spine, additional features include a reversal of the lumbosacral rhythm when straightening from the flexed position and compensatory movement for an immobile spine, such as flexion from the hips. In assigning category DRE II, the assessor must provide detailed reasons why the category was chosen.
4.19 Asymmetric or non-uniform loss of ROM may be present in any of the three planes of spinal movement. Asymmetry during motion caused by muscle guarding or spasm is included in the definition.
Asymmetric loss of ROM may be present for flexion and extension. For example, if cervical flexion is half the normal range (loss of half the normal range) and cervical extension is one-third of the normal range (loss of two thirds of the range), asymmetric loss of ROM may be considered to be present.
4.20 While imaging and other studies may assist medical assessors in making a diagnosis, the presence of a morphological variation from ‘normal’ in an imaging study does not confirm the diagnosis. To be of diagnostic value, imaging studies must be concordant with clinical symptoms and signs. In other words, an imaging test is useful to confirm a diagnosis, but an imaging study alone is insufficient to qualify for a DRE category (excepting spinal fractures).
4.21 The clinical findings used to place an individual in a DRE category are described in AMA5 Box 15-1 (pp 382–83).
The reference to ‘electro-diagnostic verification of radiculopathy’ should be disregarded.
(The use of electro-diagnostic procedures such as electromyography is proscribed as an assessment aid for decisions about the category of impairment into which a person should be placed. It is considered that competent assessors can make decisions about which DRE category a person should be placed in from the clinical features alone. The use of electro-diagnostic differentiators is generally unnecessary).
4.22 The cauda equina syndrome is defined in Box 15.1 in Chapter 15 of AMA5 (p 383) as ‘manifested by bowel or bladder dysfunction, saddle anaesthesia and variable loss of motor and sensory function in the lower limbs’. For a cauda equina syndrome to be present there must be bilateral neurological signs in the lower limbs and sacral region. Additionally, there must be a radiological study which demonstrates a lesion in the spinal canal, causing a mass effect on the cauda equina with compression of multiple nerve roots. The mass effect would be expected to be large and significant. A lumbar MRI scan is the diagnostic investigation of choice for this condition. A cauda equina syndrome may occasionally complicate lumbar spine surgery when a mass lesion will not be present in the spinal canal on radiological examination.
4.23 The cauda equina syndrome and neurogenic bladder disorder are to be assessed by the method prescribed in the spine chapter of AMA5 Section 15.7 (pp 395–98). For an assessment of neurological impairment of bowel or bladder, there must be objective evidence of spinal cord or cauda equina injury.
Applying the DRE method
4.24 The specific procedures and directions section of AMA5 Section 15.2a (pp 380–81) indicates the steps that should be followed to evaluate impairment of the spine (excluding references to the ROM method). Table 4.1 below is a simplified version of that section, incorporating the amendments listed above.
4.25 Common developmental findings, spondylosis, spondylolisthesis and disc protrusions without radiculopathy occur in 7%, 3% and up to 30% of cases involving individuals up to the age of 40 respectively (AMA5, p 383). Their presence does not of itself mean that the individual has an impairment due to injury.
4.26 Loss of sexual function should only be assessed where there is other objective evidence of spinal cord, cauda equina or bilateral nerve root dysfunction. The ratings are described in AMA5 Table 15-6 (pp 396–97). There is no additional impairment rating system for loss of sexual function in the absence of objective neurological findings. Loss of sexual function is not assessed as an ADL.
4.27 Radiculopathy is the impairment caused by malfunction of a spinal nerve root or nerve roots. In general, in order to conclude that radiculopathy is present, two or more of the following criteria should be found, one of which must be major (major criteria in bold):
- loss or asymmetry of reflexes
- muscle weakness that is anatomically localised to an appropriate spinal nerve root distribution
- reproducible impairment of sensation that is anatomically localised to an appropriate spinal nerve root distribution
- positive nerve root tension (AMA5 Box 15-1, p 382)
- muscle wasting – atrophy (AMA5 Box 15-1, p 382)
- findings on an imaging study consistent with the clinical signs (AMA5, p 382).
4.28 Radicular complaints of pain or sensory features that follow anatomical pathways but cannot be verified by neurological findings (somatic pain, non-verifiable radicular pain) do not alone constitute radiculopathy.
4.29 Global weakness of a limb related to pain or inhibition or other factors does not constitute weakness due to spinal nerve malfunction.
4.30 Vertebral body fractures and/or dislocations at more than one vertebral level are to be assessed as follows:
- Measure the percentage loss of vertebral height at the most compressed part for each vertebra, then
- Add the percentage loss at each level:
- total loss of more than 50% = DRE IV
- total loss of 25% to 50% = DRE III
- total loss of less than 25% = DRE II
- If radiculopathy is present then the person is assigned one DRE category higher.
One or more end plate fractures in a single spinal region without measurable compression of the vertebral body are assessed as DRE category II.
Posterior element fractures (excludes fractures of transverse processes and spinous processes) at multiple levels are assessed as DRE Ill.
4.31 Displaced fractures of transverse or spinous processes at one or more levels are assessed as DRE category II because the fracture does not disrupt the spinal canal (AMA5, p 385) and do not cause multilevel structural compromise.
4.32 Within a spinal region, separate spinal impairments are not combined. The highest-value impairment within the region is chosen. Impairments in different spinal regions are combined using the combined values chart (AMA5, pp 604-06).
If there are adjacent vertebral fractures at the transition zones (C7/T1, T12/L1), the methodology in paragraph 4.30 in the Guidelines is to be adopted. For fractures of C7 and T1, use the WPI ratings for the cervical spine (AMA5 Chapter 15, Table 15-5, p 392). For fractures of T12 and L1, use the WPI rating for the thoracic spine (AMA5 Chapter 15, Table 15-4, p 389).
4.33 Impact of ADL. Tables 15-3, 15-4 and 15-5 of AMA5 give an impairment range for DREs II to V. Within the range, 0%, 1%, 2% or 3% WPI may be assessed using paragraphs 4.34 and 4.35 below. An assessment of the effect of the injury on ADL is not solely dependent on self-reporting, but is an assessment based on all clinical findings and other reports.
4.34 The following diagram should be used as a guide to determine whether 0%, 1%, 2% or 3% WPI should be added to the bottom of the appropriate impairment range. This is only to be added if there is a difference in activity level as recorded and compared to the worker’s status prior to the injury.
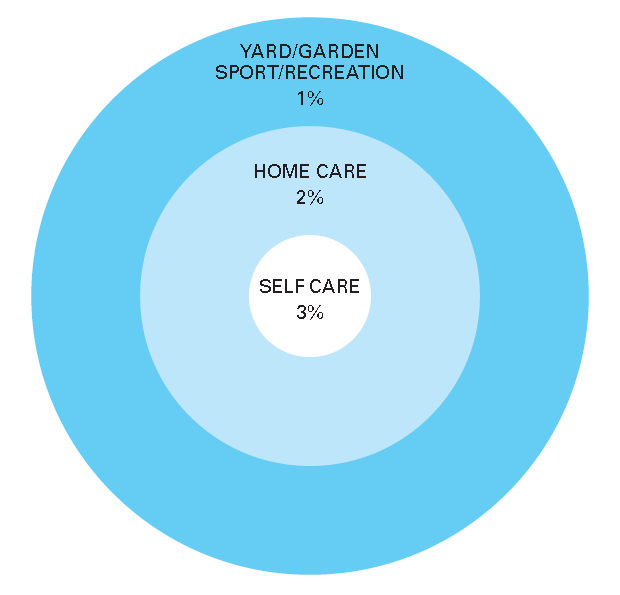
4.35 The diagram is to be interpreted as follows:
Increase base impairment by:
- 3% WPI if the worker’s capacity to undertake personal care activities such as dressing, washing, toileting and shaving has been affected
- 2% WPI if the worker can manage personal care, but is restricted with usual household tasks, such as cooking, vacuuming and making beds, or tasks of equal magnitude, such as shopping, climbing stairs or walking reasonable distances
- 1% WPI for those able to cope with the above, but unable to get back to previous sporting or recreational activities, such as gardening, running and active hobbies etc.
4.36 For a single injury, where there has been more than one spinal region injured, the effect of the injury on ADL is assessed once only.
For injuries to one spinal region on different dates, the effect of the injury on ADL is assessed for the first injury. If, following the second injury, there is a worsening in the ability to perform ADL, the appropriate adjustments are made within the range. For example, if WPI for ADL is assessed as 1% following the first injury and 3% after the second injury, then WPI for ADL for the second injury is assessed as 2%.
For injuries to different spinal regions on different dates, where there is a worsening of ability to perform ADL after the second injury, additional impairment may be assessed. For example, if ADL for a cervical spine injury is assessed as 1%, and an assessment of a subsequent lumbar spine injury determined 3% WPI for ADL, then WPI for impact on ADLs for the lumbar injury is assessed as 2% WPI.
4.37 Effect of surgery: AMA5 tables 15-3 to 15-5 (pp 384, 389 and 392) do not adequately account for the effect of surgery on the impairment rating for certain disorders of the spine. The assessor should note that:
- Surgical decompression for spinal stenosis is DRE category III (AMA5 Table 15-3, 15-4 or 15-5)
- Operations where the radiculopathy has resolved are considered under the DRE category III (AMA5 Table 15-3, 15-4 or 15-5).
- Operations for spinal fusion (successful or unsuccessful) are considered under DRE category IV (AMA5 Table 15-3, 15-4 or 15-5)
- DRE category V is not to be used following spinal fusion where there is a persisting radiculopathy. Instead, use Table 4.2 in the Guidelines
- Radiculopathy persisting after surgery is not accounted for by AMA5 Table 15-3, and incompletely by tables 15-4 and 15-5, which only refer to radiculopathy that has improved following surgery.
Table 4.2 indicates the additional ratings which should be combined with the rating determined using the DRE method where an operation for an intervertebral disc prolapse, spinal canal stenosis or spinal fusion has been performed.
Example 15-4 in AMA5 (p 386) should therefore be ignored.
Table 4.2: Modifiers for DRE categories following surgery
| Procedures | Cervical | Thoracic | Lumbar |
|---|---|---|---|
| Spinal surgery with residual symptoms and radiculopathy (refer to 4.27 in the Guidelines) | 3% | 2% | 3% |
| Second and further levels | 1% each additional level | 1% each additional level | 1% each additional level |
| Second operation | 2% | 2% | 2% |
| Third and subsequent operations | 1% each | 1% each | 1% each |
In summary, to calculate whole person impairment (WPI) for persisting radiculopathy (as per definition) following surgery:
- Select the appropriate DRE category from Table 15-3, 15-4, or 15-5;
- Determine a WPI value within the allowed range in Table 15-3, 15-4 or 15-5 according to the impact on the worker’s ADL
- Combine this value with the appropriate additional amount from Table 4.2 to determine the final WPI.
4.38 Disc replacement surgery: The impairment resulting from this procedure is to be equated to that from a spinal fusion.
4.39 Arthritis: See paragraphs 3.19 – 3.24, Chapter 3 of the Guidelines.
4.40 Posterior spacing or stabilisation devices: The insertion of such devices does not warrant any additional WPI.
4.41 Spinal cord stimulator or similar device: The insertion of such devices does not warrant any additional WPI.
4.42 Impairment due to pelvic fractures should be evaluated with reference to the following table, which replaces AMA5 Table 15-19.
Table 4.3: Pelvic fractures
| Disorder | Whole person impairment |
|---|---|
| 1. Non-displaced, healed fractures | 0 |
| 2. Fractures of the pelvic bones (including sacrum) | |
| i. maximum residual displacement <1cm | 2 |
| ii. maximum residual displacement 1 to 2cm | 5 |
| iii. maximum residual displacement >2cm | 8 |
| iv. bilateral pubic rami fractures, as determined by the most displaced fragment: | |
| a. maximum residual displacement ≥2cm | 5 |
| b. maximum residual displacement >2cm | 8 |
| 3. Traumatic separation of the pubic symphysis | |
| i. <1cm | 5 |
| ii. 1 to 2cm | 8 |
| iii. >2cm | 12 |
| iv. internal fixation/ankylosis | 5 |
| 4. Sacro-lliac joint dislocations or fracture dislocations | |
| i. maximum residual displacement ≥1cm | 8 |
| ii. maximum residual displacement>1cm | 12 |
| iii. internal fixation/ankylosis | 5 |
| 5a. If two out of three joints are internally fixed/ankylosed | 8 |
| 5b. If all three joints are internally fixed/ankylosed | 10 |
| 6. Fractures of the coccyx | |
| i. healed, (and truly) displaced fracture | 1 |
| ii. excision of the coccyx | 5 |
| 7. Fractures of the acetabulum: Evaluate based on restricted range of hip motion |
The rating of WPI is evaluated based on radiological appearance at maximum medical improvement, whether or not surgery has been performed. Multiple injuries of the pelvis should be assessed separately and combined, with the maximum WPI for pelvic fractures being 20%.

